that the medical community still fails to see
Why dizziness and unsteadiness ruin lives, confuse doctors, and demand an urgent rethink of the way healthcare systems approache balance disorders

Imagine waking up every morning unsure whether the floor beneath your feet will feel stable, whether you will be able to walk to the toilet without support. Imagine planning your day around the fear of falling, avoiding travel, crowds, stairs, and even social gatherings. Imagine being told repeatedly that “all tests are normal” while you and your surroundings appear to be unstable and life quietly shrinks.
This is not a rare story. It is the daily reality for millions of people living with vertigo, dizziness, and unsteadiness—collectively known as vestibular symptoms.
Despite being among the most common medical complaints worldwide, balance disorders remain poorly understood, either inadequately investigated or over investigated, and very frequently mismanaged. They represent one of modern healthcare’s most neglected yet disabling conditions —an epidemic that unfolds silently, without visible scars, but with devastating consequences for the sufferer.

Symptoms Are Not Diseases—But Warnings
Vertigo, dizziness, light-headedness, and imbalance are symptoms, not diagnoses. These are signals—alerts / alarms from a complex balance system that includes the inner ear, brain, spinal cord, peripheral nerves, eyes, muscles, joints, cardiovascular system, and even the psychic system. The vestibular symptoms are just the external manifestation of some underlying disease that may be a self-limiting trivial non-sinister disease or some life threatening disease with catastrophic sequlea.
Treating these vestibular symptoms as diseases and trying to suppress the vestibular symptom by anti-vertigo medications without ascertaining the underlying causative disorder is like silencing a fire alarm without looking for the fire. The consequences are disastrous. It is like trying to treat malaria or pneumonia with paracetamol.
Sadly, this is precisely what happens in most cases and is the conventional practice.

A Problem That Is Far More Common Than We Admit
Population studies consistently show that:
- Vestibular symptoms account for 5–10% of all primary care visits
- Nearly one-third of ENT and neurology consultations involve dizziness or imbalance
- Over 20% of individuals experience balance problems at some point in life
- Prevalence rises sharply with age—affecting one in three people over 60 and half of those above 80

In India alone, these figures translate into tens of millions of affected individuals. Yet the healthcare system continues to treat balance disorders as trivial inconsequential routine ailments or as manifestations of hypochondria, weakness, or general debility, rather than an incapacitating public health hazard that jeopardises the affected person’s very existence.
he Human Cost: Life Lived in Fear
The true burden of balance disorders is not captured by statistics alone. Patients often have:
- Constant and often agonising fear of falling
- Avoidance of travel and public places
- Withdrawal from social activities
- Reduced work productivity or job loss
- Persistent anxiety, frustration, and helplessness
Over time, many patients lose confidence in themselves, and more often than not in medicine, and in the medical profession itself. What begins as a physical symptom gradually evolves into emotional exhaustion and a mentally occupying psychological distress.

The tragedy is that most sufferers endure this silently—because dizziness leaves no visible disability or any external manifestations that can arouse empathy and sympathy.
The Endless Medical Carousel
One of the most distressing experiences for balance-disorder patients is the diagnostic merry-go-round
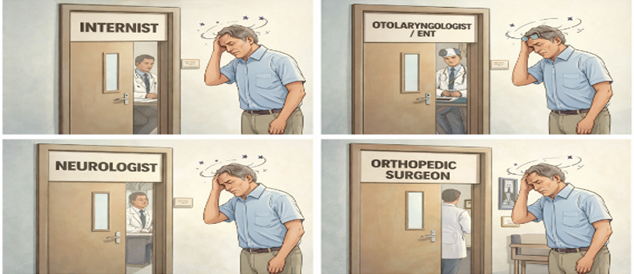
Most of the hapless patients often shuttle between:
- General physicians → ENT specialists → neurologists → Cardiologists → gastroenterologists → orthopaedic surgeons → physiotherapists → acupuncturists
Everybody benefits except the patient
Each consultation brings:
- Repeated investigations, sometimes newer ones , more often repetitions of the same old ones from newer places
- Conflicting opinions
- New prescriptions— but most usually, variations of the same medications in different brand names
The result is confusion, financial strain, and growing mistrust. Patients begin to ask:
- “Why am I not improving?”
- “Is this psychological?”
- “Do I have a brain tumour or stroke?”
- “Will I ever feel normal again?”
- “Why is the doctor treating me so casually?”
The Medication Trap
A unique but despicable feature in the treatment of balance-disorder patients is the overuse of symptom-suppressing medications.
So-called “anti-vertigo” medications that can at best camouflage some of the vestibular symptoms like head spinning temporarily are frequently prescribed for weeks, months, or even years—despite the fact that:
- They do not treat the underlying disease
- They can worsen unsteadiness and dizziness
- Long-term use may retard / delay recovery
- Current practice guidelines forbid use of such medications for more than 1-3 days

Many of these drugs suppress sensory input from the balance organs, interfering with the brain’s natural ability to recalibrate and compensate—a process known as vestibular compensation. Ironically, the very medicines meant to help patients to overcome their balance problems may keep them perpetually dizzy, and eternally unsteady. Hence they are best avoided.
Why Doctors Are Also Confused
The problem does not stem from negligence—it stems from systemic gaps in medical education and training infrastructure.
1. Inadequate Training
Neurotology —the science of balance and vestibular disorders—receives minimal attention in undergraduate and postgraduate medical curricula. Most doctors are never formally trained to evaluate balance as a multisystem functional disorder. As a result, learning for the practising clinician is basically limited to sales talks by marketing organisations selling Pharmaceutical products or Diagnostic instruments. Other than this any source of information is from fragmented and curated conference teachings meant to unscrupulously promote the promoters, and sponsors of the conference i.e., the same pharmaceurical companies and sellers of diagnostic equipment.
True expertise is difficult to attain and remains rare.


2. Misplaced Diagnostic Emphasis
Balance assessment is time-intensive and requires a huge amount of effort from the clinician in the form of detailed history taking, analysing the chronology of events , careful clinical examination involving the balance as well as the neurological systems and also assessment of psychic and cognitive status. But most busy clinics do not afford the time to do justice to a balance disorder patient. Instead, rely heavily on:
- Imaging
- Isolated vestibular tests
While vestibular testing has a role, it is frequently over-emphasised, sometimes performed without clinical correlation, and often interpreted by non-specialists who are devoid of any insight into the vestibular system. Hence the results of the vestibular function tests are very often wrong and misleading to the clinician.
Meanwhile, simpler and cheaper assessments of:
- Peripheral nerve function
- Proprioception
- Lower-limb circulation
- Sensory deficits
are commonly overlooked—even though non-vestibular causes account for most balance disorders. Vestibular disorders contribute to less than a third of the patients seeking treatment for balance related symptoms.
Balance Is a Team Effort—Not an Inner-Ear Solo
A critical misconception is that balance disorders originate solely from the inner ear. In reality, balance depends on the seamless integration of inputs from the:
- Vestibular labyrinths (inner ear)
- Proprioception (muscles, joints, feet)
- Vision
The inputs are processed in the highest echelons of the brain and involve the cognitive and the psychic systems.
In daily life, especially when the subject is standing / walking on firm ground in good lighting, proprioception (not the inputs from the vestibular labyrinths) contributes nearly 70% of balance control. Disorders affecting nerves, spinal pathways, or blood supply to the legs can severely impair balance—even when the vestibular labyrinth the inner-ear is normal.
Ignoring these contributors leads to incomplete diagnosis and misdirected/ ineffective treatment.

The Overlooked Role of Mind and Cognition
Chronic balance disorders rarely exist in isolation. They frequently coexist with:
- Anxiety and depression
- Cognitive impairment
- Impaired attention and memory
- Fear-based movement avoidance
- Agoraphobia
These are not imagined symptoms. Vestibular dysfunction directly affects brain networks involved in cognition and emotion. Treating balance disorders without addressing the concomitant psychological and cognitive health is often futile.
Rehabilitation: The Most Underused Cure
While drugs dominate prescriptions, rehabilitative therapies remain grossly underutilised.
Evidence consistently shows the effectiveness of:
- Vestibular physiotherapy
- Occupational therapy
- Structured balance training
- Cognitive-behavioural strategies
- Supervised mind-body practices
These therapies re-calibrate and re-train the brain, restore sensory integration, rebuild confidence, and reduce fear.

Crucially, they must be delivered by trained professionals, not generic exercise handouts distributed as tearaway sheets. Balance rehabilitation is a science to be delivered by trained professionals —not a tearaway sheet or a pamphlet.
Why Dedicated Balance Clinics Matter
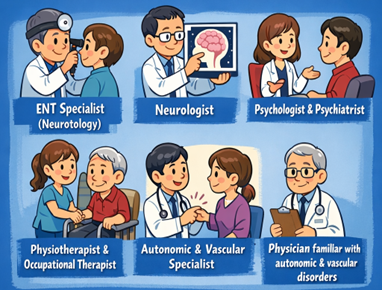
Balance disorders cannot be managed by one specialty alone. Optimal care requires a multidisciplinary model, bringing together:
- Neurotology-trained ENT specialists
- Neurologists
- Psychologists and psychiatrists
- Physiotherapists and occupational therapists
- Physicians familiar with autonomic and vascular disorders
Where such integrated clinics exist, outcomes improve, unnecessary investigations reduce, and long-term healthcare costs fall.
In aging societies, these clinics are not optional—they are a mandatory requirement.
The Price of Neglect
Failure to address balance disorders leads to:

- Preventable falls and fractures
- Long-term disability
- Loss of productivity
- Emotional suffering
- Escalating healthcare costs

Ironically, healthcare systems spend heavily on imaging and medications while under-investing in rehabilitation—the very intervention most likely to restore balance function and physical /social independence
Rewriting the Story
The widespread belief that balance disorders are incurable is wrong.
With:
- Accurate diagnosis
- Cause-specific treatment
- Multidisciplinary rehabilitation
Most patients can improve substantially—and many recover fully.
What is urgently needed is:
- Better medical training
- Public awareness
- Ethical diagnostic practices
- Expansion of specialised balance clinics
A Final Word
Dizziness and unsteadiness are not minor complaints. They are warning signals from one of the body’s most complex systems.
Recognising balance disorders as a serious, treatable, and multidimensional health issue is the first step toward restoring dignity, mobility, and confidence to millions who currently suffer in silence.
The epidemic is invisible—but easily correctable with a mix of empathy, improved social awareness, better teaching and ethical and rational medical practices.